
Treatment documentation is essential because it functions as part of the patient’s medical history, enables collaborative care between providers and authorized entities, results in a better quality of care, and more. The phrase “if it’s not documented, then it didn’t happen” might sound extreme, but in the world of healthcare-whether medical or holistic-it’s the norm. Importance of SOAP Notes and Treatment Documentation
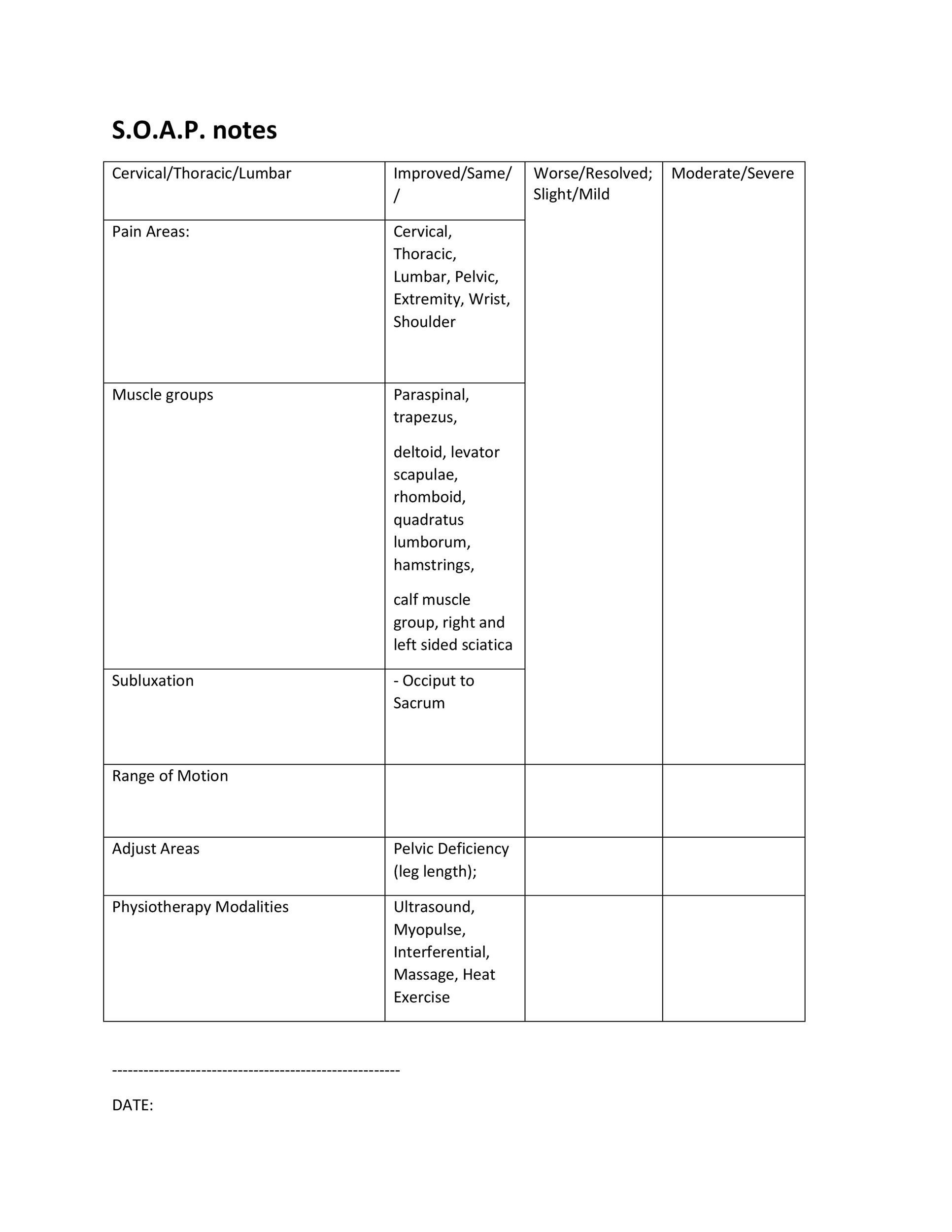
The plan section is an essential conclusion to the SOAP notes outline because it provides the appropriate next steps and pertinent information for the patient to follow in order to begin their plan for treatment.

This section might include information like: The final step in writing SOAP notes is, of course, to outline a plan of care for the patient you’re serving. Assessing the patient is helpful for other providers to review your conclusions and inform them on how best to deliver holistic care from their specialty or perspective. The assessment portion of SOAP notes is important because it provides documentation of the diagnosing process and serves as a record of your thinking. In this section, you might list whatever problems or diagnoses that patient is presenting with, in order from most to least important or severe. This third step of SOAP notes is where you bring together the subject and objective portions of your documentation and determine what might be ailing your patient. As with all medical documentation, it’s also crucial to filter out any kind of assumptions in the note-taking process each objective note should be verifiable through evidence. It’s important to distinguish between symptoms and signs in this section symptoms are considered subjective whereas signs are considered objective notes. ObjectiveĪs opposed to subjective, this second section deals with objective, unbiased facts regarding the patient’s condition. This initial section is important for illuminating how a patient’s condition is affecting them so that you can determine how best to address their pain points-both literal and metaphorical. Explain how the pain started and how it might change during the day with different movements, what makes it worse or what helps reduce the pain, etc.Describe the sensation of the pain, such as shooting, dull, cramping, tingling, throbbing, aching, etc.Rate the intensity of pain on a scale of 1 to 10.The purpose of this section is to provide context for why the patient is visiting your holistic practice and to allow the patient to put into their own words what is going on with them.ĭepending on the setting of your holistic practice and what type of treatments you offer to your patients, this section might have a few other subheadings to further elaborate on what the patient is experiencing.įor example, if you were doing a consultation for massage therapy services, you might include the following sections: This is the first section of SOAP notes and pertains to the subjective experience of the patient you’re treating this includes their feelings, perspective, and personal views as relevant to the treatment setting. Each section of this general formula is key to gathering a comprehensive report of the patient’s current experience and determining the best treatment plan. One standard form of healthcare documentation is called SOAP notes, which stands for Subjective Objective Assessment and Plan. Treatment notes are needed to keep a live record of how your patient is feeling and what plans have worked in the past or what needs to change for the future keep reading to learn more about a particular outline of healthcare documentation called SOAP notes and how they can play a role in your holistic practice’s insurance billing cycle. Healthcare documentation is a critical component for your holistic practice, both in terms of delivering great care to your patients and for insurance billing purposes-not to mention the importance of having some form of documentation in the event of a legal situation.
